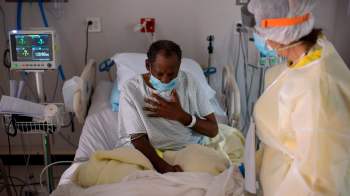
Long COVID can make work challenging. Accommodations can make a difference.
Long COVID can make work challenging. Accommodations can make a difference.

Before Brenda Currie got COVID-19, work was a huge part of her identity. She had two jobs, one as a hotel concierge in Portland, Oregon, another as a kids’ ski coach. She loved being “a high-functioning professional” in the city.
“I was leading this dynamic life in the sense that I was very fulfilled by what I did,” she said. “That was my life and my livelihood.”
But in March 2020, as the world was shutting down, she got sick. And she never fully recovered.
Months later, “I was having severe issues with my eyes and my cognition,” said Currie, who’s now 62. “There was a disconnect between my brain and my eyes, and there still is.”
She would get dizzy when she stood up, she had intense fatigue, she couldn’t focus to read or watch movies, and she eventually realized she couldn’t work, at least not like she had before.
“I was having a hard time,” Currie said. “Like I said, my career was so important to me, I was at a complete loss.”
About 7% of adults in the U.S. have long COVID, according to a recent survey from the Centers for Disease Control and Prevention. That’s almost 18 million people. For many, the illness is severe enough that it’s affecting their ability to work. One study from the Brookings Institution estimates that about 700,000 people are likely missing from the labor force because of it.
“Long COVID can cause many diverse and fluctuating symptoms, it can impact multiple organ systems, and it has no official treatments,” said Beth Pollack, a research scientist at the Massachusetts Institute of Technology who studies long COVID and other infection-associated chronic illnesses.
Some of the most common symptoms are extreme fatigue, brain fog and other neurological issues, shortness of breath, pain, and post-exertional malaise, which is when symptoms get worse after physical or cognitive exertion.
“When you talk to people with long COVID, what you hear often is a story of loss. These illnesses impact their lives so significantly,” Pollack said. “And one of the losses that really impacts people both personally in their lives and professionally and financially is that too often, they’ve had to lose their careers.”
But not everyone is sick enough that they want to or have to leave their jobs. For many, “what they really need is the right accommodations so that they are able to continue to work,” Pollack said.
Long COVID can be considered a disability under the Americans with Disabilities Act “if it substantially limits one or more major life activities.” People who have it are legally protected from discrimination and have a right to request “reasonable accommodations” at work.
What that means “really is dependent on the particular disability and an employee’s limitations,” said Katie Brennan at the Society for Human Resource Management.
“A common accommodation that employers provide is leave,” she said. “Other common accommodations could include things like telework, flex scheduling, extra rest breaks. Maybe providing some sort of equipment, like noise-canceling equipment, for instance, if someone has cognitive issues or trouble concentrating.”
Employers are required to make reasonable accommodations for people with qualifying medical conditions, as long as it doesn’t pose an “undue burden” on them.
“The onus is on the employer to demonstrate the undue burden,” Brennan said. “In most cases, an employer is going to approve an accommodation.”
About 40% of managers reported having employees with long COVID in a 2022 survey from the nonprofit Kessler Foundation, and of those, nearly 60% said their employees received accommodations.
In more than half of cases, workplace accommodations don’t cost an employer anything, according to the nonprofit Job Accommodation Network. In most other cases, it’s a one-time cost of $300 or less.
But not every employer knows their responsibilities, and not every employee knows their rights under the ADA.
When Brandon Beck tried to go back to his job as a mechanical engineer after having COVID in late 2020, he struggled.
“I ended up with some extreme fatigue that I’m still dealing with,” he said. “Body tremors daily that I’m still dealing with, headaches that I’m still dealing with, brain fog, which is getting much better.”
Before getting sick, Beck, 40, had been working 60-hour weeks and was frequently on the road. After, he could barely stay awake for more than a few hours at a time.
One doctor told him he had post-COVID syndrome, but he said, “when I’d tell anybody about it, of course, a lot of people were in disbelief.”
This was late 2020, early 2021, and long COVID was still so new that, at least in Beck’s circles near Flint, Michigan, “nobody knew anybody that had been affected by it, including my HR guy that, at the time, totally did not believe anything I had to say,” he said.
The only accommodations his employer was willing to offer him was a full 40-hour week in the office rather than on the road. When Beck proposed working from home, his employer refused. He ended up taking unpaid leave, and while he was out, he said, he was let go.
“It is 100% a stigmatized diagnosis,” said Dr. Monica Verduzco-Gutierrez, who directs the long COVID clinic at UT Health San Antonio. “I’ve even had some patients tell me, ‘Don’t give me that diagnosis, or don’t write it down because of how people are going to look at me.’”
Even finding a doctor who knows about long COVID, or takes it seriously, can be a challenge, and those that do are in high demand.
“Some patients, I will see them, maybe it’s a year after they’ve been dealing with COVID,” Verduzco-Gutierrez said. “The waiting list to get into clinic can be several months.”
And often, employers require documentation from a doctor to approve accommodations at work, especially if a disability or illness isn’t visible or obvious, which is often the case with long COVID and other complex chronic illnesses like myalgic encephalomyelitis/chronic fatigue syndrome and fibromyalgia.
“I think there’s challenges because still, there is not a lot of clarity in the diagnosis,” Verduzco-Gutierrez said. “If someone had a traumatic brain injury, at one point, they had an MRI that showed they had damage to their brain. For long COVID, we don’t have a biomarker.”
Meaning there’s no test a doctor can run that shows someone has long COVID.
As long as that’s the case, “it’s much harder to diagnose, and it’s much easier to dismiss,” said Doron Dorfman, an associate professor at Seton Hall Law School. “Doctors are gatekeepers for disability law in a lot of ways, specifically for reasonable accommodations.”
If someone is unable to find a doctor who believes them and is willing to fill out the necessary documentation, an employer may refuse to approve accommodations at work.
For Amy Blackstone, a sociology professor at the University of Maine, “it’s been a battle every step of the way.”
Ever since getting COVID four years ago, she’s been living with daily fatigue, vertigo, nausea, migraines and brain fog that make teaching in person, and traveling the state to do fundraising like she used to, impossible.
Her primary care doctor refused to consider the possibility that it was long COVID, and largely because of that, Blackstone said, “it took a year and a half for me to get a diagnosis” and find a doctor who would fill out paperwork for her to get accommodations at work.
In that time, she used up months of paid time off that she had accrued over the 20 years she had been working at the university. Now, she has an accommodation to work fully from home, doing research and teaching online.
Even though it’s been a struggle, Blackstone said, “I know how much luckier I am than so many other people.”
Beth Pollack, at MIT, recently co-wrote a piece for the Harvard Business Review, “Long COVID at Work: A Manager’s Guide,” and in researching it, “we heard many stories, from people losing their careers, to people being able to not only keep working, but also be promoted and really thrive in their careers,” she said. “And the differences between these stories are often that people were able to receive accommodations that were tailored to their specific symptoms, so they got the exact support they needed.”
For Mindy Jackson, a vocational services specialist for the Department of Labor and Industries in Washington state, that means being able to work from home and have a flexible schedule.
Jackson has received a slew of diagnoses since she had COVID four years ago — chronic fatigue syndrome; dysautonomia; postural orthostatic tachycardia syndrome, or POTS; and rheumatoid arthritis. They make a full-time, in-office job challenging.
“I would really like to be able to work consistently 40 hours a week, but what I’m learning is I can’t really work 40 hours a week and have quality of life,” she said. “And so it’s just trying to find that balance.”
Both her doctor and her employer have been supportive as she tries to find that balance, she said, which has made it possible for her to keep her job.
For Brenda Currie in Portland, it took a while to find work she could do with all the physical and cognitive limitations she now has because of long COVID.
The first couple of jobs she tried, in customer service, ended up being too much; she quit, without ever asking for accommodations or telling anyone that she has long COVID.
“Because it’s invisible,” Currie said. “And I felt like it would work against me. Because I’ve always been a really valuable employee, very capable and competent. But I became really aware that I had a serious issue at hand, and I was going to have to deal with it.”
Eventually, when she was ready to try working again, she applied for a part-time job at a new retail store opening in town, and got it.
“And it was very clear from the beginning that I was really struggling,” she said. “And I had to sit down with my manager and say, ‘I have long COVID, and I’ve been very sick.’”
It was hard for her to do. But her managers have been accommodating. She has worked with her, scheduling Currie for shorter shifts and telling her that any time she needs to take a break, she can.
It still takes all of her energy to work just 15 hours a week, Currie said, but “being back at work, and being part of the economy, and also being out in the community and helping people, it’s really powerful.”
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.