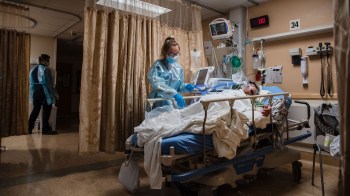
Hospitals are short-staffed and running out of beds. Again.
Hospitals are short-staffed and running out of beds. Again.

It’s happening again. With COVID-19 cases surging in many states, a growing number of hospitals are running out of beds in intensive care.
“It’s not just the physical bed, it’s the staffing that goes along with it … the nursing, the respiratory therapy, the pharmacists and the physicians,” said Dr. Jorge Caballero, who co-founded Coders against COVID, an organization that analyzes COVID data.
At least a few hospitals in almost every state are dealing with critical staffing shortages, according to recent data submitted to the Department of Health and Human Services. The problem is most acute in the South and Southwest.
“What I’m seeing is that in states like Alabama, Arizona, Louisiana, Missouri, more than one out of five hospitals are reporting that they have a critical staffing shortage,” Caballero said.
Our Lady of the Lake Regional Medical Center in Baton Rouge, Louisiana, is one of those hospitals struggling with staffing.
“The biggest reason is absolutely because more people are in the hospital,” said Dr. Catherine O’Neal, the chief medical officer at Our Lady of the Lake. “The volume is just something we’ve never seen before.”
It is a mix of new COVID patients, recovered COVID patients coming back with complications and people who put off other medical care because of the pandemic.
“So those who are sick from other things got sicker, and so now they need an additional level of care,” O’Neal said. “And so the combination is just a sicker population of people who need more hospital care than they did before.”
There are also fewer people on staff to take care of all of them, partly because of burnout — a year and a half into COVID, more and more health care workers are deciding they simply can’t take it anymore.
“We have seen our health care providers just move on to nonhospital care venues because they’re tired of the pandemic,” O’Neal said.
Finding new staff is also more challenging than it’s ever been because every hospital is competing for the same people.
“It’s almost like a game of Hungry Hippo,” O’Neal said. “There’s only a certain amount of nurses, physical therapists and respiratory therapists in the world, and now everybody’s volumes are much higher because of COVID.”
And they’re not going down.
“Every hospital I’ve ever worked in has had a pandemic preparedness or a disaster preparedness plan, but never for this length of time,” said Dr. Kavita Patel, a primary care doctor in Washington, D.C., and a fellow at the Brookings Institution.
Many hospitals were already contending with some level of staffing shortages before the pandemic, but in the past when demand spiked — maybe during a bad flu season, for example — they could generally hire temporary nurses and staff up quickly.
“But there’s not as many of those temporary nurses to go around because every hospital needs them,” Patel said. “I can’t even think of a time when almost every single state had some set of needs.”
Nursing is the most critical need for most hospitals now, but not the only one.
“The shortages go all the way down the line, even to custodial staff,” Patel said. “You never realize how much you desperately need custodial staff until you have to turn around to COVID room.”
At hospitals around the country, particularly in the South, patients are feeling the backlogs. They are waiting longer in the emergency room to be seen, and in some cases, longer at home for an ambulance to come when they dial 911.
In Alaska, it hasn’t quite hit that point, but it is still “a very challenging situation up here,” said Jared Kosin, the president and CEO of the Alaska State Hospital and Nursing Home Association.
Summer is always a busy time for hospitals in Alaska, he said, “because we get outside, we’d like to go do things. So you have higher incidences of trauma, and other things like that.” Now, on top of that, COVID cases are surging again.
When a hospital is short-staffed and can’t hire all the nurses and doctors it needs to meet demand, one of the first steps it will often take “is canceling procedures, and then redeploying those staff,” Kosin said. “So if you need people working on ventilators, you cancel surgeries and redeploy anesthesiologists, assistants, so on and so forth.”
Just recently, hospitals in Anchorage had to delay nonessential surgeries temporarily to relieve some of the pressure.
If COVID-19 keeps surging, Kosin is worried things could get even worse. That could be curbed, but only if a lot more Alaskans get vaccinated — soon.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.