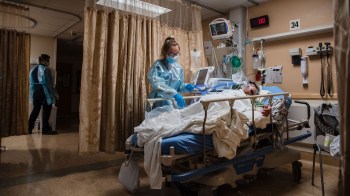
“How long do I plan to stay? As long as necessary.” — a home health care worker in quarantine
“How long do I plan to stay? As long as necessary.” — a home health care worker in quarantine

While frontline health care workers in hospitals across the country are dealing with COVID-19, home health care workers are trying to help their clients stay out of emergency rooms by bringing health care support to the elderly and people with disabilities.
In some cases, they are choosing to quarantine with their clients.
Anna Castillo is a personal care attendant who has been working with her client, a 74-year-old woman with debilitating arthritis, for more than two years. Castillo helps her out of bed in the morning, bathes her and prepares meals.
In recent weeks, Castillo’s shifts have gone from six hours a day to 24/7.
“I’m just keeping everything under control, checking to see if she’s OK, if she doesn’t have a temperature, making sure that she takes her medication and all of the vitamins possible and avoids the world outside.”
Castillo lives just north of Boston in Chelsea, Massachusetts, with her husband. But in mid-March, she decided to move in with her client in South Boston to reduce the risk of carrying COVID-19 into her client’s home.
Even though her paycheck doesn’t reflect her new schedule, she said she felt she had no other choice.
“How long do I plan to stay? As long as it’s necessary. She wouldn’t be able to survive on her own,” Castillo said.
As a personal care attendant, Castillo is considered a direct-to-consumer home health worker and she’s paid by Mass Health, the state’s Medicaid program. She makes about $15 dollars an hour, pays out of pocket for her own health benefits and says she’s still only getting paid for six hours of work a day.
Castillo is one of more than two million home health workers in the U.S., according to PHI, a national advocacy nonprofit.
According to Rebecca Gutman with the service workers union 1199SEIU, the home health care workforce is made up largely of immigrants and women of color.
“It’s heroic work during normal times, and during the pandemic there’s a lot more fear among home care workers as they’re going to work,” Gutman said.
Unlike Castillo, many of these workers are still commuting. They often take public transportation, live in substandard housing and get by living paycheck to paycheck.
“You have one vulnerable population caring for another vulnerable population,” Gutman said, “and then they’re going into the homes of people with disabilities and elders, and doing so without personal protective equipment.”
The service workers union is collecting and distributing masks and gloves for home health workers but, said Gutman, it’s slow going, due in large part to the national shortage.
In the meantime, Castillo said, home health workers and personal care attendants are advised to screen clients daily for fever, avoid unnecessary travel and wash their hands frequently.
“Given the ramp-up of positive COVID-19 cases in nursing homes right now, probably the safest place for elders and people with disabilities to be right now is in their homes,” said Gutman. But, she stressed, that means home health care workers must have a way to protect themselves.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.