An ICU nurse describes the exhaustion of working on COVID’s front lines
An ICU nurse describes the exhaustion of working on COVID’s front lines

Across the country, COVID-19 continues to surge and hospitals are filling to capacity. Los Angeles is currently experiencing some of the highest numbers of cases in the country. And yet, for most Angelenos, life looks the same as it has for much of the pandemic.
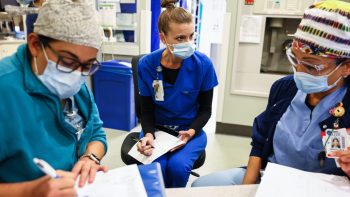
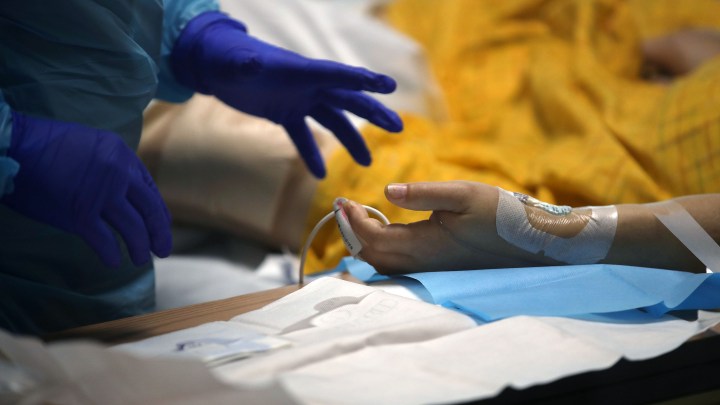
Health care workers on the front lines, however, are coming up on one year of watching patient after patient die alone in a hospital bed. And it is taking its toll on their mental health.
Tatiana Molinar works as an ICU nurse at Providence Saint John’s Health Center in Santa Monica, a city adjacent to Los Angeles. So when her mom tested positive for COVID in April, she was able to get her transferred to her unit. Molinar helped her mom get access to experimental drugs and treatments that weren’t available in most hospitals. But ultimately, Molinar said, it wasn’t enough.
“I honestly don’t think that there’s anything that could have saved her except for her not getting sick,” she said.
In August, Molinar said, she felt overwhelmed by her mom’s death. And her husband was furloughed from his job, so she was taking on extra shifts as a surge of her patients were dying of COVID.
She said she felt a disconnect from the people outside her work who didn’t seem to know what it’s like to deal with COVID firsthand.
“People have no idea how ugly it is,” Molinar said. And she said many of her co-workers have turned to alcohol or antidepressants to cope with stress — “people who were fine before.”
In a recent survey of health care workers, 93% said they were experiencing elevated levels of stress, and 76% said they were physically and emotionally exhausted.
“Nearly 40% of health care workers did not feel like they have adequate emotional support, and that was even higher for nurses, about 45%,” said Maddy Reinert, senior director of population health at Mental Health America, the organization that produced the study.
That data seemed to be playing out for Molinar, as one by one, most of her friends left the intensive care unit. Today, Molinar said, most of the nurses she works with are from out of state.
“We have a lot of travelers that can earn more in LA, so they leave their states where wages are lower,” she said.
Molinar has been vaccinated. On Jan. 7, she received the second of two shots to protect her against COVID-19. While she is grateful, she said she doesn’t really feel a sense of relief yet.
“I am a little afraid that I still could be potentially transmitting the virus to folks in my community who aren’t getting the vaccine as early as I am,” she said.
According to the Centers for Disease Control and Prevention, authorities “don’t yet know whether getting a COVID-19 vaccine will prevent you from spreading the virus that causes COVID-19 to other people, even if you don’t get sick yourself.”
Still, Molinar said that for the first time since the pandemic began, she feels like there is definitely hope on the horizon.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.