How tech connects older people with mental health services as COVID-19 isolates
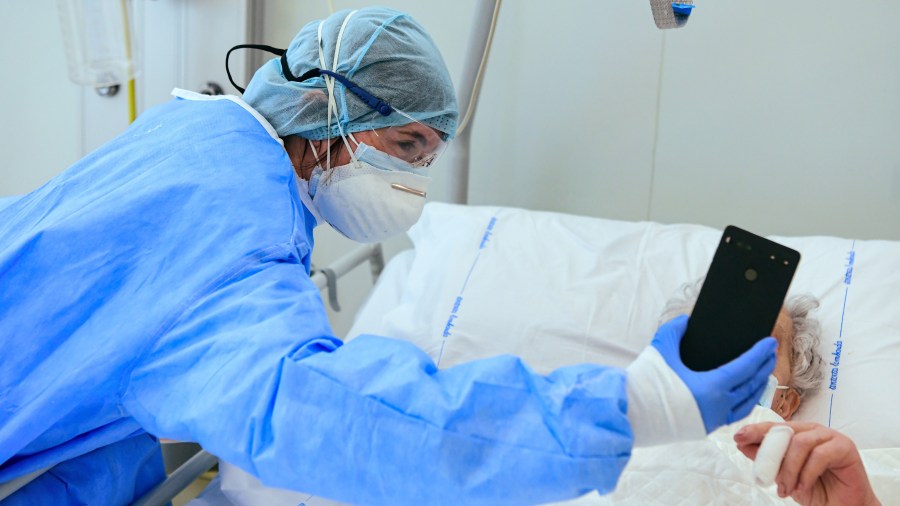
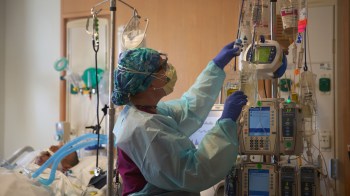
People over 65, and those in nursing facilities, are at a much higher risk of severe illness from COVID-19. And with mandated social distancing, it means they can’t have typical visits with family and friends, which makes mental health care really important. This is prompting facilities that usually rely on in-person counseling to shift to remote options. But telehealth can have its own complications.
I know this because my sister, Dr. Nichole Adams-Flores, is one of the people navigating that transition. She’s a supervising psychologist for CHE Behavioral Health Services, and she works at several nursing facilities in and around New York City. I brought her on to talk about it. The following is an edited transcript of our conversation.

Nichole Adams-Flores: First of all, we’re trying to make sure people are able to social distance from one another. So it’s not always ideal for us to take someone out of their room, wheel them through hallways where there’s lots of other people doing things and into a private room. To that end, we’re bringing the telehealth platform to our patients, [which] is happening via tablet or phone. What’s been really nice is that the rules around telehealth have altered a little bit so that the insurance companies are supporting multiple different ways that we can connect to a person. Telehealth [has] gone from just the computer screen and a person talking to a doctor via computer to also including a telephone call.
Kimberly Adams: What does that look like for different patients?
Adams-Flores: For example, I’m allowed to use WhatsApp, FaceTime or any type of video platform to conduct a session. Pre-COVID-19, there would be a prescribed way or a prescribed platform to use, and that was the only one you’d be able to use to conduct a service. Now, they’re letting us do anything we can do to make sure people get the mental health services that they need in a way that’s effective.
Adams: What does that mean for patient privacy? Are these things HIPAA [Health Insurance Portability and Accountability Act] compliant or secure for what are very sensitive conversations?
Adams-Flores: That’s been a big topic of conversation, and I don’t think people have the answers yet. When you go and meet with a patient, you ask their permission to use whatever platform you have to move forward with the conversation. If the patient gives their consent, we move forward at this point. But the conversations about privacy and HIPAA are an ongoing conversation that literally we’re having conversations about daily — and supervision and in discussion with insurance companies. These platforms aren’t traditionally the way that mental health services are delivered, and I don’t believe they were created for that purpose. To that end, now that we’re using them in this way, it’s almost like we’re working backwards a little bit. We’re using the platform for a different purpose other than what it was intended for, and now we’re trying to make sure that those platforms will ensure patient privacy.
Adams: What about quality of care, though? Is that compromised or enhanced at all by these changes?
Adams-Flores: One of the drawbacks to a telehealth platform is there isn’t the ability for human interaction in the way that you could in a counseling session. There’s something to be said for just being in the presence of another person. There’s definitely something different about it. It feels a little more distant, a little more cold. When we’re able to provide those in-person counseling sessions, many times, now, a part of that session includes being able to chat with family members. It’s wonderful that we have technology to introduce into those counseling sessions, because many of the people in our nursing facilities who are receiving care don’t have smart technology.
Adams: How could technology, and I’m talking about the devices and the software here, provide a better experience for this group?
Adams-Flores: It would be nice if software companies would be thoughtful about all the types of populations that might want to use software to do a traditional job. There’s a learning curve that goes along with any type of new technology, and somebody that might be cognitively impaired — due to a stroke or a brain injury — sometimes that technology is really hard for them to learn or begin to use in a way that’s meaningful.
Adams: In this whole interaction, you’re talking about people, some of whom know that they are at the greatest risk of serious illness or death from COVID-19.
Adams-Flores: Yes, which contributes to an exacerbation of mental health issues that they’re already struggling with. Anxiety is through the roof. Depression is just overwhelming. When you’re not able to contact or be in touch with your family members in a way that you’re used to, it really contributes to the sense of hopelessness and being overwhelmed with a sense of “Am I ever going to get better? Will my life ever be the same?” One of my patients is a Holocaust survivor. She’s in her late 90s. She was talking to me about how she really thought she was a resilient person surviving the Holocaust, coming through the experience, having a family around her all the time that loves her. And now that she is isolated from them, alone in her room most of the day, for her, she’s saying for her it’s almost like reliving wartime experience that she’s feeling so isolated. She actually had her granddaughter that was visiting her from out of town, and we were able to connect via WhatsApp. As a clinician, you feel like you’ve become desensitized to some types of emotions, but even in this session, I found that I was tearing up and crying when she saw the way that technology could really connect her to her family in a meaningful way. Now, mind you, I was holding the phone and I had to touch all the applications to make it happen. Her hands were trembling as she was crying, blowing kisses to her granddaughter, great-granddaughter, actually. It was so worth it to see how it really made an impact in a positive way. After we finished, her being able to see her family, she said, “Please come back next week. I have a list of people I’d like to be in touch with.” It was a really nice way that we were able to have technology in our session that really supported her feeling more connected to family.

Related links: More insight from Kimberly Adams
Mental Health America hosted a webinar a couple of weeks ago looking at the mental health of older Americans during the increased social isolation of the coronavirus pandemic. It warned that loneliness, depression and anxiety can contribute to a lot of other health problems. It also includes a lot of resources for how to help or get help.
There are also mental health resources from AARP and the Diverse Elders Coalition. And there’s a helpline for older people and their caregivers with COVID-19 information in different languages, including English, Spanish, Cantonese, Japanese and Korean. That’s provided by the National Asian Pacific Center on Aging.
The future of this podcast starts with you.
Every day, the “Marketplace Tech” team demystifies the digital economy with stories that explore more than just Big Tech. We’re committed to covering topics that matter to you and the world around us, diving deep into how technology intersects with climate change, inequity, and disinformation.
As part of a nonprofit newsroom, we’re counting on listeners like you to keep this public service paywall-free and available to all.
Support “Marketplace Tech” in any amount today and become a partner in our mission.