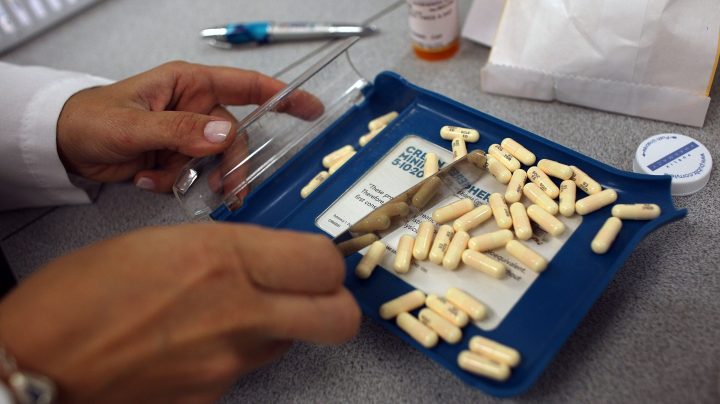
The free market is failing us on antibiotics

Researchers at Harvard Medical School in 2016 recorded a now-famous demonstration with E. coli bacteria — a species often behind recalls of contaminated food.
“What we ended up building was basically a petri dish, except that it’s two feet by four feet,” explains Harvard Medical School’s Michael Baym in a video about the experiment.
The giant petri dish had different sections with different levels of an antibiotic. Part of it had no antibiotic, then a lethal level, then 10 times the lethal dose, 100 times, 1,000 times. When the researchers released the bacteria into the dish, they grew like a white wispy cloud right up until they hit the antibiotic. Then, they stopped cold.
“Then, a mutant appears on the right,” Baym goes on. “It’s resistant to the antibiotic, it spreads … when these mutants hit the next boundary they too have to pause and develop new mutations to make it into 10 times as much antibiotic.”
This repeats itself as the bacteria evolve to survive more antibiotic. After 11 days, the bacteria are thriving in 1,000 times the lethal level, and the black petri dish has become white. The video is quite simply the evolution of one of humanity’s greatest nemeses, caught on film.
Some 35,000 people in the U.S. die every year from antibiotic-resistant infections; that figure is 1.3 million globally.
“Bugs always win,” is a refrain Dr. Evan Loh likes to repeat. “If you continue to use older antibiotics, they get stronger and stronger and stronger.”
This is happening. Existing antibiotics are becoming less effective as bacteria evolve, but the market that should be developing new antibacterial medicines is failing.
And the World Health Organization says the pipeline for antibacterial treatment is insufficient. There are only eight antibiotics in the late stages of development and only three are considered innovative, according to the Antimicrobial Resistance Industry Alliance. Of the new antibiotics in preclinical trials any given year, about a third are discontinued.
“You really need a buffet table of novel antibiotics to be able to actually stay ahead of the innovation curve that’s needed as bacteria evolve and develop resistance,” Loh said.
In addition to being a physician, Loh is CEO of Paratek Pharma, which is the producer of an FDA-approved antibiotic called Nuzyra for pneumonia and skin infections.
“We unfortunately are the exception whereas we should be the norm,” he said.
Paratek has benefited from government programs, and its antibiotic fits a particular critical need. It also comes at a premium, though the company has offered the antibiotic for free to people without insurance or any other way to get it.
Paratek has also been working on developing and commercializing its new antibiotic since the ’90s — and has spent $1 billion doing so. It is one of only a handful of biotechs developing new antibiotics.
“Large pharma companies, which traditionally have developed these antibiotics, have largely exited both the research space and the commercialization space,” Loh said.
Some have filed for bankruptcy, shares have tumbled in others. “Investors have walked away from this sector,” he added.
They’ve walked away because the current economics often don’t work.
“What’s different about antibiotics is that when you develop a really good one, it shouldn’t be used very much,” said James Anderson, chair of the AMR Industry Alliance. Antibiotics, especially new ones, should not be put in every medicine cabinet, but rather used only when absolutely necessary.
“Sales are low and, indeed, when you look at the average sales of all the antibiotics that have been launched in the last 10 years or so, it’s less than $50 million a year — which is not enough to sustain ongoing operations in many companies, let alone to give a return on investment,” Anderson said.
In many cases, it costs hundreds of millions of dollars more to develop an antibiotic than will be earned from it.
“It takes 10 to 20 years and $560 [million] to $700 million to develop an antibiotic, by some estimates,” said Jocelyn Ulrich, deputy vice president of medical innovation policy at PHRMA, a pharmaceutical industry trade group. Other estimates are much higher — $1.5 billion.
“The return is in the hundreds of millions, max,” she said, and often not enough to make it worth the expense. And all the expense does not guarantee approval by the FDA.
Additionally, pharmaceutical companies can’t necessarily count on having a global market, because bacteria are evolving and spreading in different ways around the world.
“The particular pathogen that I have to deal with may well be different from the pathogens that a colleague in Greece or Lebanon or Korea has to deal with,” explained Dr. Vance Fowler, professor of medicine at Duke University.
The market failure is accelerating, said Ulrich. “Twenty years ago, around 18 of the largest biopharmaceutical companies were involved in AMR product research and development, and now we’re down to about five major players. The majority are small biotechs.”
It’s the invisible hand versus Darwinian evolution. And right now, evolution is winning.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.

















