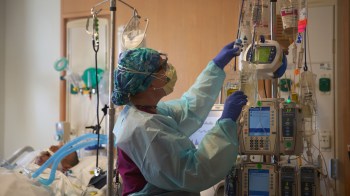
Pandemic price gouging complaints raise staff tensions with traveling nurses
Share Now on:
Pandemic price gouging complaints raise staff tensions with traveling nurses

Like most traveling nurses right now, Pamela McNairy of Mississippi says she’s making more money than she ever thought possible. She’s working in a Southern California COVID unit, getting $10,000 a week before taxes.
But that’s working 13-hour shifts, overnight, five nights a week.
“We’re the ones who are actually doing the real patient care and keeping these people alive,” she said. “I’m telling you, it’s hard.”
So it doesn’t sit well with McNairy that the American Hospital Association is calling for price gouging inquiries into staffing agencies, citing reports of pay rates tripling from before the pandemic. Nearly 200 members of Congress have signed on in support.
Hospitals are crying foul over the high prices they have to pay traveling nurses during an escalating staff shortage.
“When you see price increases that are two or three or more times what they were before the pandemic, it’s fair to at least investigate about whether or not these companies are price gouging,” AHA general counsel Mindy Hatton said on a media conference call.
Some legislators have proposed pay caps. A Pennsylvania lawmaker is even trying to cap travel pay in nursing homes; nurses report health systems are trying to set limits, too.
The corporate claims of financial stress are not helping strained staff relations.
“The ones who make the decisions, they don’t walk into a COVID patient’s room,” McNairy said. “They’re not risking their lives. They’re not away from home.”
McNairy has four kids and a husband in Mississippi, and she’s been away from her family for much of the pandemic.
Traveling nurses have always been paid more for their flexibility and experience. But hospitals say the going rate, which is often above $120 an hour, has ballooned beyond what they can afford. In the first quarter of this year, the Henry Ford Health System in Michigan plans to spend $50 million on what CEO Wright Lassiter calls “crisis labor.”
“That is the exorbitant labor cost related to the recent inflation in travel and contract nursing to supplement our staffing,” he said.
Of its 9,000 nursing jobs, Lassiter said 1,000 positions were open in January. Many nurses have left bedside roles during the pandemic to travel to COVID hotspots, given the much higher pay, creating a vicious cycle where their replacement will likely have to be a pricey traveler rather than a lower-paid permanent staffer.
Rural hospitals have had particular trouble holding on to their bedside staff, and not just nurses. West Tennessee Healthcare’s hospitals in the small communities of Camden and Bolivar lost half of their respiratory therapists who specialize in ventilating COVID patients to staffing agencies, according to CEO Ruby Kirby.
“We cannot compete with the salaries that they are offering to recruit additional staffing,” she said.
CEOs have been careful to focus their criticism on staffing agencies — not nurses themselves — especially since many executives still make considerably more money. For example, Lassiter made $5.2 million in 2019 or roughly $100,000 a week, according to the most recent tax filings.
Hospital CEOs point out that traveling nurse agencies tack on an extra 30% or more for overhead and profits. Toby Malara, the American Staffing Association’s vice president of government relations, said an agency’s cut is paying for real expenses like recruiters and nurse training, not just profits.
And staffing firms are providing a way for nurses to work hard for three-month periods with high pay and then take a break.
“We know that if nurse staffing agencies weren’t around, we’ve heard from these nurses, that they might be out of the business altogether,” Malara said.
The American Nurses Association predicts another 500,000 nurses will be retiring this year and projects the need for 1.1 million new nurses to avoid a nursing shortage.
Nurses are organizing what’s being billed by some as a “million nurse march” in Washington, D.C. on May 12. McNairy said she’s hoping to fly across the country to be there so nurses can be heard.
“I can tell you this,” she said. “If they mess with our money, we’ll walk out.”
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.