Rural hospitals, short of staff, brace for omicron
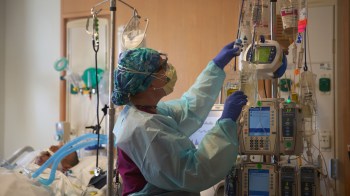
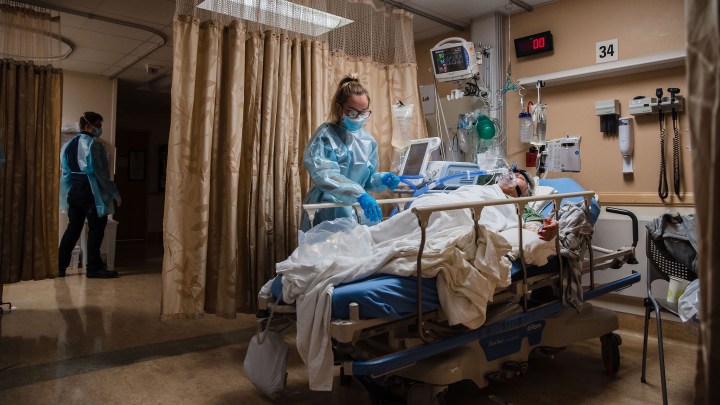
Rural hospitals, short of staff, brace for omicron

Hospitals in the U.S. are struggling to stay staffed up. Many were short of workers even before the pandemic caused an exodus of doctors and nurses from the field.
Now, the more transmissible omicron variant is sending some of the remaining workers home, and hospitals are running out of backup plans — particularly in rural areas.
Vermont was already in dire need of health care workers, even before the pandemic drove many into early retirement and other careers, according to Jeff Tieman with the Vermont Association of Hospitals.
“Our workforce is shrinking and stressed, you know, at a time when we need it to be growing and resilient,” he said.
In New Mexico, more than half of hospitals face critical staffing shortages.
“The amount of physical, mental, emotional fatigue is showing,” said Deborah Walker with the New Mexico Nurses Association.
Many care providers have left the state’s overwhelmed rural hospitals on traveling nurse contracts “to pay off student loans and to command a higher salary,” she said.
With the national shortage of health care workers, small, rural hospitals are having a hard time hiring, said Joanne Spetz with the Institute for Health Policy Studies at the University of California, San Francisco.
“Just because of their locations, their financial situations are often more precarious,” she said.
And with the rise of omicron and many rural communities’ low vaccination rates, “you’re looking at potentially a large number of people coming into the small hospital and possibly having staff out sick,” Spetz said.
That can force rural patients to travel hundreds of miles for care.
“The chances of finding that next hospital, and on time if it’s an emergency, will be decreasing,” said Christine Porter, a professor of public health with the University of Wyoming. “It’s a great time to not need a hospital.”
She said the state’s health care workforce is bracing for omicron.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.