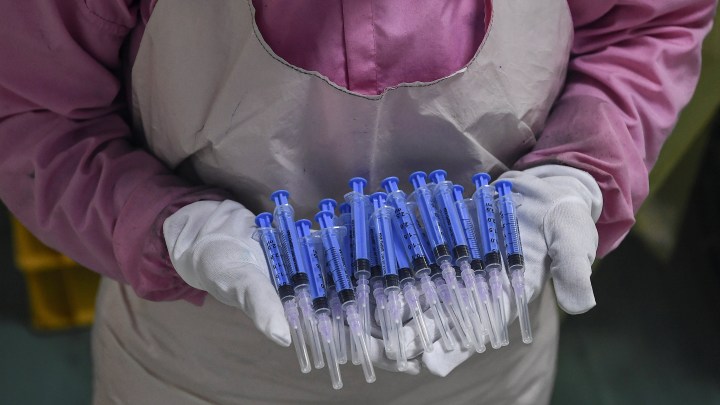
We need a centralized, global strategy to prevent another COVID pandemic, epidemiologist says
We need a centralized, global strategy to prevent another COVID pandemic, epidemiologist says

COVID infection numbers have fallen in the United States, but other parts of the world, like India and Brazil, have seen spikes, partly due to vaccine supply shortages.
The situation has led the World Health Organization to suggest that richer countries share their surplus vaccine supplies as soon as possible.
It’s far from the global vaccine equality that experts like Dr. Larry Brilliant, CEO of Pandefense Advisory, who helped stop the smallpox epidemic, wanted to see last year.
For Brilliant, it’s only underlined the need for a centralized, global plan that would strategically deliver vaccines to those who need them most.
“We have to figure out vaccine-saving strategies that will allow us to use the vaccine that we can make, the good vaccine that we can make, and distribute it in as speedy and effective way as we can,” Brilliant said in an interview with “Marketplace Morning Report” host David Brancaccio. “And to do those things, you need a global campaign, a global program.”
These structures already exist to some degree, such as WHO’s Global Outbreak Alert and Response Network, but Brilliant is thinking of something akin to a global response unit proposed by the Independent Panel for Pandemic Preparedness and Response.
The following is an edited transcript of Brilliant’s conversation with Brancaccio about potential vaccine-saving strategies, what a centralized global COVID organization should have and the funding needs involved in preventing another COVID pandemic.
David Brancaccio: Now here we are opening up, talking about taking masks off in so many places. If you move your gaze beyond our borders, though, different situation.
Larry Brilliant: Yes, it’s a Dickensian moment. It’s the best of times here and the worst of times in India. And it is a tale not of two cities, but of two countries, probably two different worlds.
Brancaccio: I mean, there’s this move, right, to open source coronavirus vaccine technology. How significant do you think that would be to help the rest of the world wrestle this virus to the ground?
Brilliant: Well, I think, you know, changing the intellectual-property rights, helping other countries manufacture vaccine is a part of the solution. But by far, it’s not, it’s not even the most important part. In smallpox eradication and polio, we managed to get those vaccines manufactured all over the world. But if you think that, with all the new variants that are being created, that everyone’s going to need to get two doses and then perhaps a booster every year or two, and you think of this as a three-year program, you’re talking about 20 to 40 billion doses of vaccine that will have to be delivered to capital cities in 200 countries. And then once they get there, that’s when the hard part begins. That’s when the global vaccination program becomes national campaigns with jeeps and distribution systems. And we’re not in the fifth or sixth inning. We don’t know if we’re playing a doubleheader or if it’s going to be a seven-game series.
Brancaccio: So when you hear that, for instance, Denmark and Norway, they have high domestic vaccination rates in those countries, but they say they don’t want to use their AstraZeneca vaccines anymore, and they are pleased to ship them to other countries. Is that the spirit you want to see? Or is that a little odd, sending the cast-off vaccine?
Brilliant: Well, first, I don’t think it should be cast off. It may turn out that the least amongst us is the most valuable. It may turn out that the AstraZeneca actually turns out to be one of the better primer vaccines, if we think about this idea that you’re going to have one or two original vaccines. In Africa there have only been 20 million people vaccinated, so the huge need for vaccines there outweighs, I think, the problems that AstraZeneca has had. But leave apart which vaccine it is. We need such a huge quantity, that we do need to understand what vaccines can mean, rapidly all over the world. And if we’re looking at quality, we have to look really hard at the Chinese vaccines and the Russian vaccines. Those have shown inconsistent results far more challenging, I think, than AstraZeneca.
Brancaccio: You know, with the global challenges at this scale, I mean, in looking at India, what has to happen now? I mean, we’ve done incredible innovation on vaccine, but you want something much larger to be done.
Brilliant: Yeah, so I’d like a dose of humility and a dose of courage. And I think a little bit of history. We’ve been successful in eradicating smallpox. That was a mostly 35-country campaign. And polio, we were down to two countries. That’s a campaign that’s lasted decades and has cost tens of billions of dollars. We need to understand what we face. We cannot eradicate this disease, David, because it exists in a dozen animal species. We will not get to global herd immunity. Mass vaccination, which is so laudable, it is inadequate because we can’t get to herd immunity. We have to figure out vaccine-saving strategies that will allow us to use the vaccine that we can make, the good vaccine that we can make, and distribute it in as speedy and effective way as we can. And that means we need to look to the lessons of ring vaccination, just-in-time vaccinating. I hear that the U.K. is moving some vaccine to one city that has been the recipient of the Indian variant, that kind of focused vaccination. It’s different than outbreak control. Those are really, in the end, vaccine-sparing or vaccine-saving strategies. And to do those things, you need a global campaign, a global program. Can you tell me where the global campaign office is for COVID? And what agency’s running it and who the leader of it is?
Brancaccio: Well, I know. I’ll be naive, I’ll say, doesn’t the World Health Organization do that for a living?
Brilliant: Well, the World Health Organization has done that extraordinarily successfully in the past with smallpox and polio. But right now, there are so many different actors and particularly we’re in an era different than we were in smallpox eradication, where it seemed like after the Second World War, all the world came together in some kind of a centripetal force. Now we’re in centrifugal forces, and nationalism is predominant. I don’t think that countries are able or willing to accept that kind of centralization, yet we need to have it. So no, I don’t think that it’s clear. The report that came out from the Independent Panel is excellent. It doesn’t name, shame or blame. That was, unfortunately, a restriction on it. That would have been more emotionally satisfying. But what it has done is proposed a system where there’s a task force for global health threats that’s created by the General Assembly of the United Nations, and then that oversees what a new, more empowered WHO would do. We’re gonna be having that conversation for quite a while. But we need a new structure. We need a global program. We need to share best practices and observe and learn from our failures. And we need to manufacture an awful lot of vaccine and create the way to deliver it that uses the least vaccine by focusing on the people most likely to get the next case of the disease, as we’ve learned from Ebola two years ago in the Congo and certainly as we learned from smallpox eradication.
Brancaccio: Maybe it’s online in the modern world, but you have like a situation room that says, here’s a hot spot, Country X. Country Y has got extra vaccine, let’s get it there in 24 hours. That kind of situation?
Brilliant: Yeah. What good does it do to vaccinate me for a third time? I’m living on a hill in [San Francisco]. That vaccine is not effectively used compared to sending it to India or having it made in India and resurrecting the Serum Institute of India, which historically has been the major producer of vaccine in the world. We need to be looking at this through a global lens. It’s satisfying to see the amazing job that the Biden administration has done in getting so many people vaccinated so quickly, but it is only 40% of the country that is fully vaccinated. It’s a little bit alarming to think that after 40% of the game is played, you want to declare victory, especially when the rest of the world or so many parts of the rest of the world are on fire. The funeral pyres in India and Nepal put the lie to any belief that we may have that we’re there yet.
Brancaccio: So start with, you think, the United Nations structure to come up with a new global organization for rapid response and for vaccine resource allocation?
Brilliant: No, I actually think we have a wonderful organelle inside of WHO called GOARN— Global Outbreak [Alert and] Response Network. It’s a terrific organization. It’s not well-funded, WHO structure is complex. This new report by an independent commission headed up by two former heads of state, Ellen Sirleaf and Helen Clark, former prime minister of New Zealand and Ellen Sirleaf is the former president of Liberia, it’s a serious report. It really requires paying attention for 85 pages and all the annexes. It’s a really good beginning. We need to focus on having a global campaign. Look, we had a great global campaign against smallpox, we’ve had a wonderful campaign against polio, we’re down to two countries. Let’s learn from that and create a global, unified campaign against COVID.
Brancaccio: Because in your view, if we don’t this thing ain’t going away.
Brilliant: Well, let’s just take a look at some of the variants. There’s a mathematical thing here. The more cases, the more viruses. If we’ve had 130 million cases reported, we probably had a billion cases. And each one of those cases have had tens or hundreds of billions of viruses. And every one of those viruses wants only one thing, and that’s to replicate. And with every one of those multiple trillions of replications, there are some mutations. And some of those mutations are bad for the virus, and they die out. Some of those mutations are good for the survival of the virus, and they become variants. And some of those variants become variants of interest, variants of concern or variants of high consequence, the highest category that WHO has. A very high consequence for us, David, would it be like 2020 over again, almost like a new disease. The vaccines would have to be reformulated, we’d have to get revaccinated. The vaccine might clobber our countermeasures, our immunotherapy. It may elude our tests. We have already variants that do each one of those things, in part. I’m not saying that’s a high probability. I think it’s a low probability, but it’s a nonzero probability. And what does the world do when we have even a small chance of repeating the horror of 2020?
Brancaccio: All right. So draw from an existing unit in the World Health Organization, and figure out how to resource it and organize it in a way that it can be most effective.
Brilliant: That’s one of the things the Independent Panel suggests, is that WHO — and I must tell the listeners, the entire budget for the World Health Organization is just about the same as the San Francisco medical expenses each year. I mean, it’s a tiny budget, and the fight between China and the United States over WHO and who’s going to fund it and the structure of WHO, where it takes its marching orders from an annual assembly of 200 countries, those have got to be addressed, and this Independent Panel report does, in fact, begin to address them.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.


















