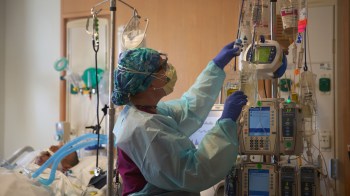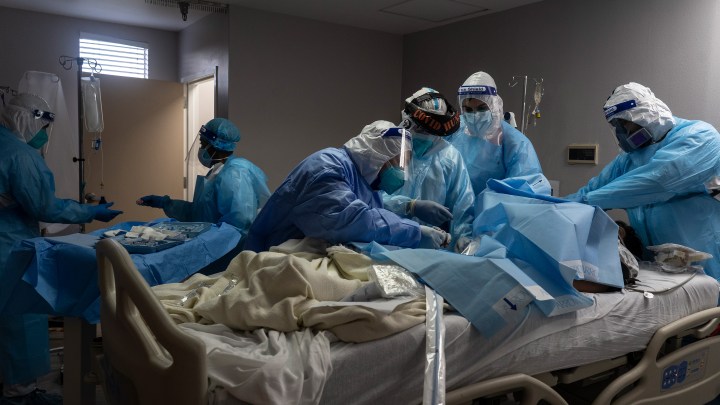
In the U.S., around 1 in 5 hospitals have a critical shortage of staff
In the U.S., around 1 in 5 hospitals have a critical shortage of staff

Robert Hancock, a physician who treats patients in Texas and Oklahoma, has seen firsthand what it’s like when overwhelmed hospitals experience COVID-19 outbreaks among staff.
“I personally tried to transfer a patient and basically tried everywhere within 150 miles and nobody had available ICU beds,” Hancock said.
He’s forced to keep patients in emergency rooms and ask overwhelmed ER nurses to look after three times the number of patients he said they should.
As the pandemic surges and more medical professionals themselves are coming down with COVID, nearly 1 in 5 hospitals in the country report having a critical shortage of staff, according to data from the Department of Health and Human Services.
John Henderson, president and CEO of the Texas Organization of Rural & Community Hospitals, said staffing problems are getting worse.
“Particularly when you go west and northwest in Texas, they’re having fits with COVID outbreaks among their staff nurses,” he said.
Another problem for hospitals whose staff contract the virus is that COVID patients often need ventilators and urgent care for a long time.
“It’s not your normal two-day hospital stay and then you turn the room over,” Henderson said. “It’s 10 days, two weeks in some instances where they’re in-patient with intensive staffing and equipment needs.”
One of the knock-on effects of staff shortages is that people who have other medical needs are being asked to wait.
“If you’ve been waiting for a few months to get in to have that funny lump that’s been seen in your breast cared for or your circulatory system needs repair, all of those things are urgent and concerning to Americans,” said Nancy Foster, vice president of quality and patient safety at the American Hospital Association.
She says hospitals are doing what they can to adapt — cross-training and redistributing work to different personnel — but the strain on staff isn’t going to let up anytime soon.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.