Anesthesia providers turn to opioid alternatives during surgery
Anesthesia providers turn to opioid alternatives during surgery

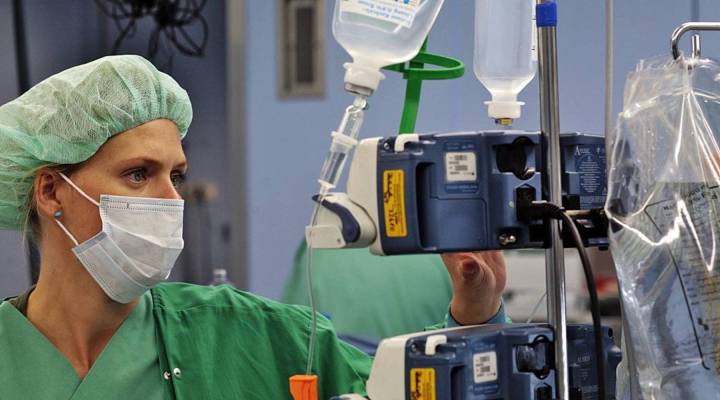
A medical team in blue scrubs crowds around the operating table during a knee surgery at West Covina Medical Center, east of Los Angeles. Most of the team are staring at the patient’s torn meniscus, but Julia Harris is watching his vitals to see if he needs more drugs to stay unconscious.
“So, he’s not sensing any of the discomfort from the surgery,” said Harris, a certified registered nurse anesthetist.
In school, Harris learned to administer fentanyl, an IV opioid, along with the anesthetic. But today, she’s using something called a nerve block instead, injecting a numbing agent into tissue around the knee to cancel the pain associated with the surgery.
This method can require more training and follow-up, and some insurance providers won’t pay for it. But Harris said her patient will be less groggy, and that means a shorter hospital stay.
“With all of our surgeries today, we haven’t needed to give any opioids at all.” Harris said.
Doctors are prescribing fewer opioid painkillers, as the medical establishment tries to deal with the current opioid epidemic. The focus has been on primary care doctors treating chronic or acute pain, but almost every patient who receives anesthesia receives fentanyl, an IV opioid more powerful than heroin.
So, anesthesia providers — who control patients’ pain during a surgery — are increasingly looking to non-opioid alternatives in the operating room.
“The opioid epidemic is really driving it,” said Tom Baribeault, a nurse anesthetist from Kentucky who founded the Society of Opioid Free Anesthesia this year. “We’re getting more and more patients that are coming in who have been addicted to opioids saying, ‘look, is there any way that we can do this without any opioids, because I don’t want to risk relapsing?’”
A Stanford University study also found that having surgery increases the risk of becoming a chronic opioid user. That’s largely because of the supply of painkillers patients are sent home with, but Baribeault said addiction can start with anesthesia, because patients can quickly become tolerant to the opioids used, and then need way more to manage their pain after surgery.
“You can’t say like, ‘Oh, these ones that I’m giving while we’re in the operating room, that’s not contributing to it,” Baribeault said. “It all contributes.”
Coming up with alternatives is tricky. Nothing kills pain like opioids, but it’s possible to use a combination of methods before and after surgery, like nerve blocks, drugs similar to Novocain, even Tylenol to get the desired effect. But those alternatives have been slow to catch on.
“It’s just very convenient to give a pill,” said Dr. Paul White, former chair of the University of Texas Southwestern Medical Center. “And our society is geared towards quick and easy solutions.”
Techniques like nerve blocks and other alternatives to anesthesia can be unfamiliar, time consuming, and pricey.
“But to me, that price is very small compared to the cost of the current opioid epidemic,” White said.
That cost, which includes health care, criminal justice spending and lost productivity, was estimated at $78.5 billion as of last year.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.