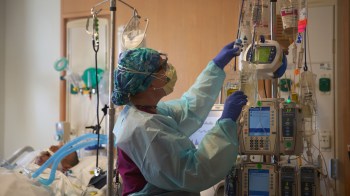
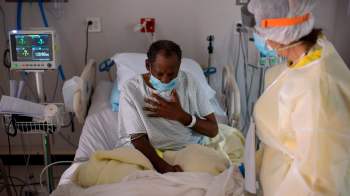
Better training for better end-of-life care
TEXT OF STORY
Kai Ryssdal: As we told you yesterday, there is a huge cost to dying in this country. Billions of dollars are spent every year on care for patients during the last two months of life. It’s not like anybody’s talking about withholding medical intervention that would offer comfort or a cure. But the problem is that studies show a significant number of the drugs and treatments given to terminally ill patients don’t have much effect on how long or how well those patients live out their lives. But there is another approach, offering more comfort at lower cost.
Marketplace’s Caitlan Carroll reports.
Caitlan Carroll: Most Americans say they don’t want to take extraordinary measures during the last few months of life and that they’d prefer to die at home. But three-quarters of Americans die in a nursing home or a hospital. Many of them dependant on machines to keep them alive. The costs, both emotionally and financially, can be huge. There is a movement now to do things differently. The first step? Listen to the patients.
Sonya Christianson: Our first question is always — well what do you want? What are you hoping for? What are you expecting? And then to gear our care around that question.
Sonya Christianson is a doctor in family medicine. She’s also completing a year-long fellowship at the Institute for Palliative Medicine at San Diego Hospice. Palliative medicine is a growing specialty that emphasizes working with chronically and terminally ill patients to plan their care. Palliative care teams are often made up of nurses, doctors, social workers and other specialists. They coordinate treatments and talk to patients about the risks and benefits of different approaches. The focus is on comfort, not cure.
Hospital worker 1: Who’s your next patient?
Hospital worker 2: In 110.
The San Diego Hospice is one of the largest non-profit hospices in the country. Although most patients are treated at home, there are about a dozen patients here in the hospice.
Hospital worker 3: So we just wanted to say hello, and I was wondering what questions you might have for us as a team.
Carlos sits up in bed as Christianson and the rest of the team file in. Carlos is in his mid-thirties and has a new baby. He also has terminal cancer. When he came to the hospice, Carlos had a breathing tube and was in pain. He says he is more comfortable now and is taking fewer medications. He’s breathing on his own, and he talks with his team regularly about his options.
Carlos: It’s been great, the attention, the nurses, the staff — they are very dedicated. I mean, I click a button and seconds later they’re here.
Charles Von Gunten: Is that different than other places?
Carlos: It’s different, yeah.
Charles Von Gunten is provost here. He leads the trainees in a discussion once they leave Carlos’s room.
Von Gunten: So can I pick on some of you who are training? What strikes you about this case?
Christianson: He said that if things don’t work out, he has the goal of just spending as much time as possible with his wife and child. And so to actually think about that and to think of an alternative to pursuing his chemotherapy is really a big deal, I think.
No one on the palliative care team advised Carlos to stop his chemotherapy. But in this setting, he’s had a chance to think about his disease and how he wants to approach treatment. Chemotherapy can be grueling. He wants to be lucid and feel well enough to enjoy time with his family.
Rosemary Gibson is the author of “The Treatment Trap.” She says too often patients end up on a train where all the momentum heads toward more treatment, even when it’s futile.
Rosemary Gibson: Palliative care is creating an option for people to get off that train, to not even got on that train if they choose not to. Not just at the end of life, but also earlier in the course of illness.
A study published in the Archives of Internal Medicine found that hospitals with palliative care programs reduced costs by about $2,000 to $5,000 per patient. Patients are treated by teams, so there are fewer mistakes. Fewer tests and treatments are ordered, and hospital stays tend to be shorter.
Gibson: We’ve seen dramatic growth in the number of hospitals with palliative care programs from about 10 in the mid-nineties to about 1,400 now, which is astonishing growth in a very short period of time.
Not everyone is moving so quickly. Many people are not familiar with palliative care or they misunderstand it as a fast track to death. Medical students aren’t required to study it, and many doctors feel they’ll be seen as giving up on a patients if they call for a palliative consult.
Doctor Gary Pasternak says there was a time when palliative care would have been the right answer. He had a patient named Julie who was dying of AIDS.
Gary Pasternak: She had had about all of the treatment that she could stand.
Pasternak realized he had been trained to cure but not care for the dying. After a spending a year studying palliative care at the San Diego institute…
Pasternak: I possess skills now that I didn’t have then. So there’s a lot of things I could do different. You know, Julie wherever you are. I’m really eternally grateful to her.
A number of states are crafting bills that would support more end-of-life counseling and palliative services. These efforts may give patients in the future more say over how they live before they die.
In San Diego, I’m Caitlan Carroll for Marketplace.
Ryssdal: Caitlan visited the Institute for Palliative Medicine at San Diego Hospice this spring. Her trip was part of a California Endowment Health Journalism Fellowship, a program of The Annenberg School for Communication & Journalism at USC. Carlos, the patient she spoke with, died not long after her visit. We’ve got resources about palliative care on our website, Marketplace.org.
There’s a lot happening in the world. Through it all, Marketplace is here for you.
You rely on Marketplace to break down the world’s events and tell you how it affects you in a fact-based, approachable way. We rely on your financial support to keep making that possible.
Your donation today powers the independent journalism that you rely on. For just $5/month, you can help sustain Marketplace so we can keep reporting on the things that matter to you.